Penetrating Wounds of the Foot
 Penetrating wounds of the horse’s hoof are quite common with farrier nails and joinery screws being the most frequent cause. When a sharp object has penetrated the horse’s foot, it can potentially cause damage to the sensitive tissues and structures inside. Depending on the depth and location of entry, the penetration can result in very serious damage, and so a penetrating foot injury should always be carefully assessed by a vet.
Penetrating wounds of the horse’s hoof are quite common with farrier nails and joinery screws being the most frequent cause. When a sharp object has penetrated the horse’s foot, it can potentially cause damage to the sensitive tissues and structures inside. Depending on the depth and location of entry, the penetration can result in very serious damage, and so a penetrating foot injury should always be carefully assessed by a vet.
The equine foot is comprised of hoof wall, sole and frog. Once the hoof wall or sole has been penetrated, the consequences will depend on what structures are damaged. The frog is the softest part of the foot and is prone to penetrating injuries. As the frog has deep grooves (or sulci) on either side, sharp objects can become wedged, before potentially being driven further into the foot.
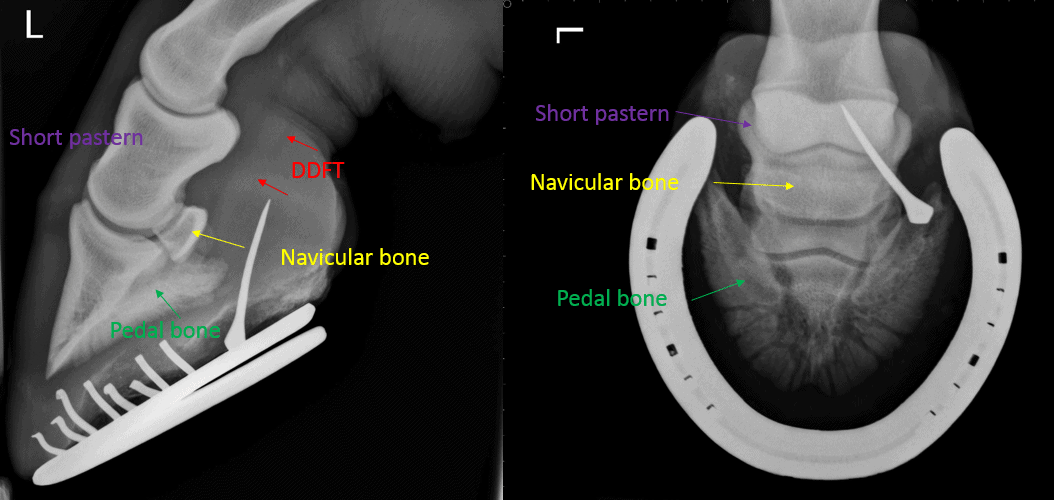
The horse’s foot contains two very important synovial structures, the coffin joint and the navicular bursa. If either of these structures are penetrated, potentially life-threatening synovial bacterial infection almost always occurs. Prompt assessment of penetrating foot wounds should therefore be performed to assess the site, depth and angle of penetration.
The navicular bursa, is only about 3 cm from the sole; in a pony it is even less. Therefore, a short nail does not have to penetrate very far to reach the bursa. If bacterial infection develops in the navicular bursa or the coffin joint (or both) then there can be disastrous consequences. The body’s immune system, in its attempt to eradicate the infection, also damages the synovial structures themselves, for example destroying the smooth surface of cartilage. In a matter of just a few days, the combination of bacterial infection and inflammatory response can cause such extensive damage to a synovial structure that a horse will be lame for the rest of its life, even with treatment, and in such situations the horse often needs to be put to sleep.
If a nail extends deeper into the foot, it can come into contact with the pedal bone. If there is sufficient force of penetration, the pedal bone is damaged and becomes infected (septic pedal osteitis). Bacterial infection can “eat away” at the bone causing serious problems and treatment is not straightforward, as antibiotics find it very difficult to penetrate infected bone. Usually the entire puncture wound tract must be pared away and the pedal bone scraped away back to healthy bone. Obviously, this procedure has a long recovery time as healthy tissue must repair the hole made in the foot.
Tetanus from any penetrating foot injury is a potentially fatal disease that is extremely difficult to treat, however it is preventable by vaccination (see Vaccination page)
In most situations it is better to leave the nail in place, as long as the horse is not standing on it, driving it deeper into the foot. Try to keep the horse calm, hold the foot up if necessary, and call out one of our vets with an xray machine, as an emergency.
If the nail has only penetrated a short distance into the soft tissues of the sole, the nail is removed, and the entry tract is pared out and enlarged to ensure any pus can drain from the infected site. The tract is drained with iodine, and possibly antibiotic saline and a poultice is placed, to keep the wound clean and draining. Tetanus cover might be given if needed, and possibly antibiotics.
If deeper structures are suspected to be involved, our vet may decide to take radiographs before they remove the nail. This will tell them exactly where the nail has gone and which structures have been damaged by the nail. Bony damage may need surgical treatment and prolonged antibiotics. If the navicular bursa or coffin joint are shown to have been penetrated, the horse will need to be referred as soon as possible to an Equine Hospital for possible further MRI of the foot, and to surgically flush out the synovial structure.
Penetrating Wounds of the Foot Read More »








